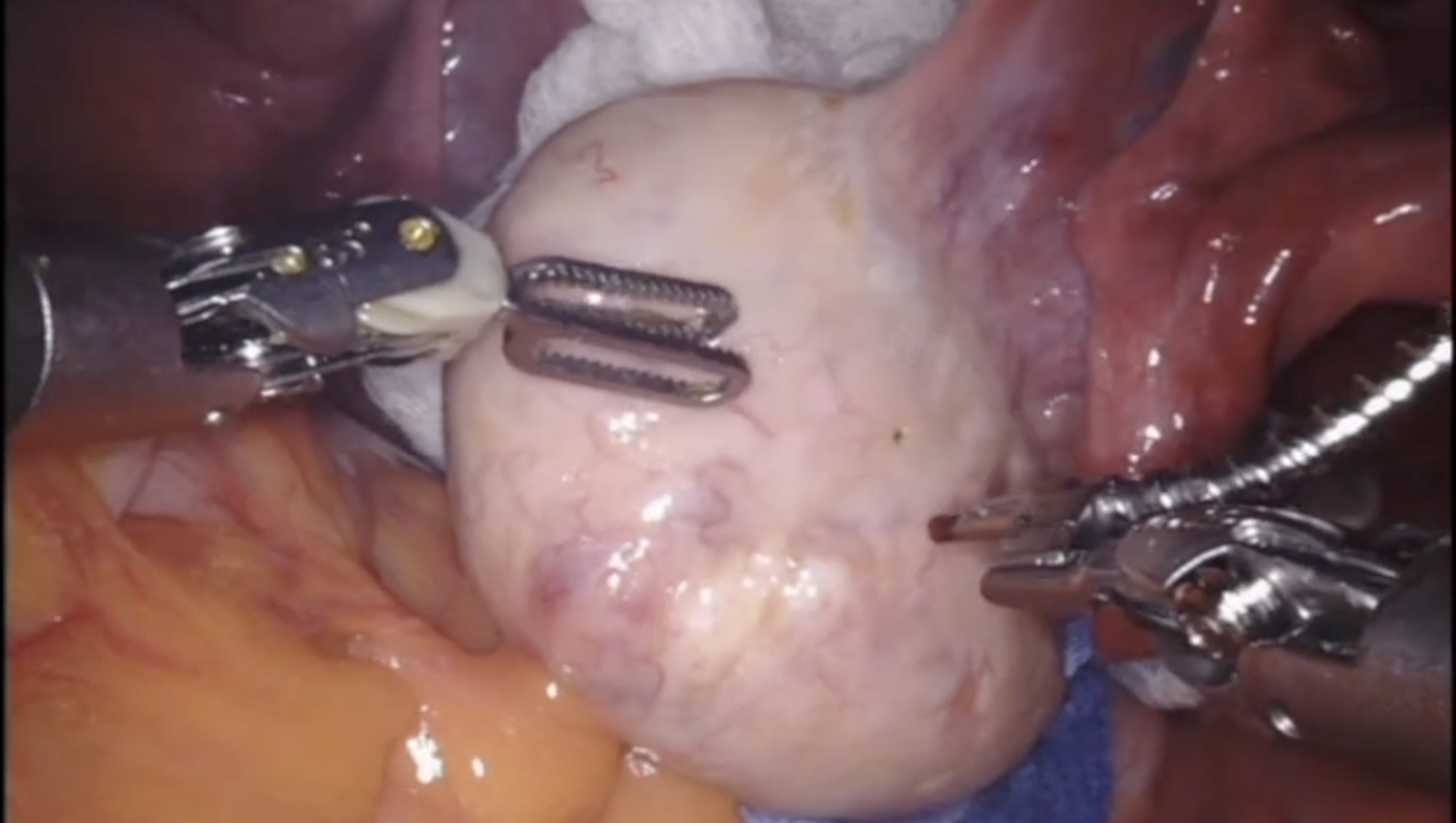
History
In 1935, Drs. Stein and Leventhal described 108 surgical cases in which 95% of the women treated with wedge resection resumed regular menstrual cycles. Moreover, 85% of those women who desired to conceive did so following the surgery. Unfortunately, the technique used to perform the surgery led to adhesion formation around the ovary and its very delicate neighbor, the fallopian tube. This was felt to hinder patient’s fertility, and therefore the ovarian wedge resection subsequently fell out of favor as a primary therapy for patients with polycystic ovaries.
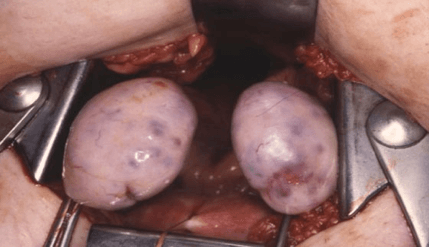
Other Treatments
Years later, the drug clomiphene citrate (Clomid) appeared on the scene and became the treatment of choice for women suffering from infertility related to polycystic ovarian syndrome, despite significantly lower pregnancy rates compared to wedge resection. Then in the 1990s with the advent of laparoscopy, a procedure known as, “laser drilling” became popular in treating this condition. As with ovarian wedge resection, laparoscopic laser drilling eliminates a portion of the central or stroma of the ovary. And while it can be effective, several studies have shown that the burning of the surface of the ovary with the laser leads to adhesion formation. It is also difficult to control precisely how much of the stroma, or center of the ovary, is destroyed making the results of ovarian drilling somewhat unpredictable.

The Preferred Solution
After developing advanced adhesion prevention techniques, researchers at the Pope Paul VI Institute for the Study of Human Reproduction in Omaha, Nebraska, have seen excellent pregnancy rates following ovarian wedge resections. Furthermore, with the advent of robotic surgery, what once required a large abdominal incision can now be accomplished through tiny laparoscopic ports. The robotic laparoscopic ovarian wedge resection allows us to perform what has always been the gold standard in treating polycystic ovarian syndrome. The robotic technology and the adhesion prevention techniques developed now make this a very powerful tool in the treatment of this devastating condition. During this procedure, we remove a wedge shaped segment of each ovary. Then using special microsurgical techniques, we sew the edges of the ovary back together in such a way as to prevent scar tissue formation.
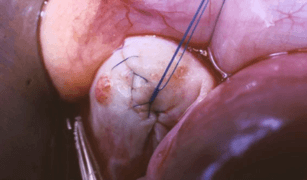
Our Process
Contrary to many other fertility specialists, we perform a comprehensive evaluation to detect all signs of disease followed by a plan to treat any abnormalities discovered. Outside of fertility, this is the way medicine is practiced. Sadly, most fertility specialists today view the absence of pregnancy as the disease itself. They respond with a plan to make the woman pregnant, typically by utilizing IVF, or IUI, or some other intervention, never taking the time to determine and then address the underlying cause or causes of the couple’s infertility.
The Procedure
A robotic laparoscopic ovarian wedge resection requires approximately one hour and is performed on an outpatient basis, typically requiring patients to be away from work no more than 5 to 7 days. The surgery is performed in the pre-ovulatory or, “pre-peak” phase of the cycle. Since the procedure is performed to treat a recognized disease, that is, polycystic ovarian syndrome, it is typically covered by most insurance plans.
The Results
Following robotic laparoscopic ovarian wedge resection, in our practice we routinely see dramatic improvement in patient’s symptoms. Lowered testosterone values, improved fasting insulin levels, and normal, spontaneous menstrual cycles, are commonly seen. Patients also often began ovulating spontaneously or respond much better to ovulation inducing medications following the surgery.
As with any surgical procedure, there are inherent risks and you should be well informed of those risks before deciding to proceed. If a patient with documented polycystic ovarian syndrome is not responding to ovulation-inducing medications, robotic laparoscopic ovarian wedge resection may offer the best opportunity to achieve pregnancy.